Pancreatic Neuroendocrine Tumors: Slow-Growing and Often Curable
By Pamela L. Kunz, MD, Associate Professor of Medicine (Oncology); Yale School of Medicine HealthDay Reporter | Copyright © 2022 HealthDay. All rights reserved.
MONDAY, June 19, 2023 (HealthDay News) -- Pancreatic cancer is often considered a death sentence, typically aggressive and usually caught late, but there is one type of pancreatic cancer that is far more treatable.
While over 90% of pancreatic cancers are adenocarcinomas, the most aggressive and deadly type, pancreatic neuroendocrine tumors (NETs) are usually slow-growing and can often be cured by surgery alone. Though these less aggressive tumors are rare by incidence (the number of patients diagnosed per year), they are more prevalent than pancreatic and gastric adenocarcinoma combined (the number of patients alive at a given time). Because of that, pancreatic NETs represent a larger public health problem than believed.
What is pancreatic cancer?
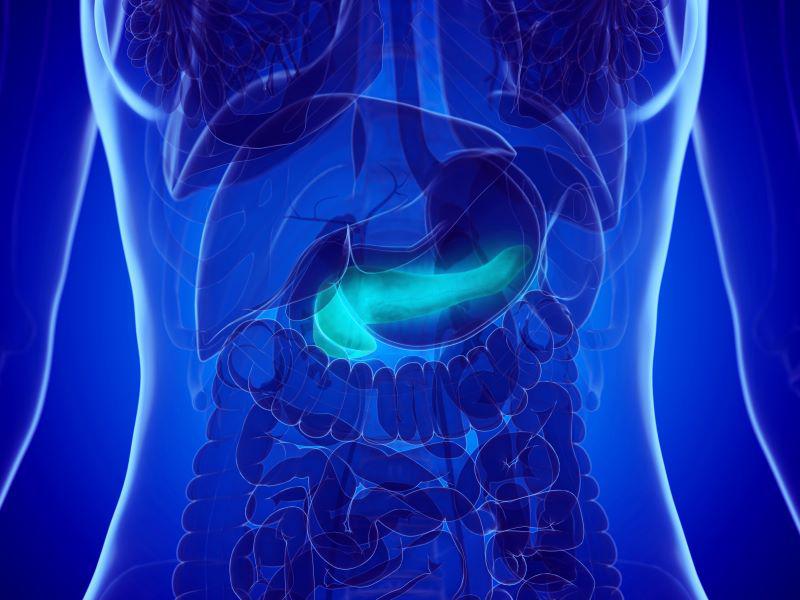
The pancreas is a large gland found in the abdomen, located behind the stomach. It is responsible for making digestive enzymes and hormones that control blood sugar levels. Pancreatic cancer forms when cells in the pancreas grow uncontrollably and spread. Pancreatic cancer can originate in the exocrine cells (the cells that make the digestive enzymes) or endocrine cells (the cells that make hormones).
Pancreatic cancer types
The majority of pancreatic cancers (90%) originate from the exocrine cells of the pancreas and is called adenocarcinoma; the remaining 10% of pancreatic cancers is comprised of several rare subtypes and includes cancer that originates from the endocrine cells, called neuroendocrine tumors.
The multiple subtypes of pancreatic cancer are all very different in terms of symptoms, risk factors, treatment and prognosis. Pancreatic NETs are often slow-growing compared to adenocarcinomas and have a better prognosis overall.
Patients have a high rate of cure and patients with metastatic pancreatic NETs can often live for many years with a “chronic cancer.” There are several important features of pancreatic NETs that physicians use to tailor treatment decisions including: stage, grade and differentiation (markers of cancer cell division and aggressiveness), hormones produced by the cancer, and presence or absence of somatostatin receptors (a special marker on the surface of the NET cell).
Pancreatic cancer symptoms
There are no screening tests for pancreatic cancers. Symptoms are often non-specific and can include fatigue, weight loss, nausea, vomiting, pain, jaundice (yellowing of skin), and new-onset diabetes. Some pancreatic NETs also produce hormones that can cause unique symptoms of hormone excess.
What causes pancreatic NETs?
We do not know what causes most pancreatic NETs. A minority of patients have a genetic predisposition. For certain patients, genetic testing may be recommended. There are no other known risk factors for developing pancreatic NETs.
Treatment for pancreatic NETs
The treatment for pancreatic NETs includes multiple options such as surgery, somatostatin analogues (a hormone treatment), chemotherapy, targeted therapies and peptide receptor radionuclide therapy (a form of targeted radiation). The best way to determine the optimal treatment for a given patient is through a multidisciplinary team, like those I work with at the Yale Cancer Center and Smilow Cancer Hospital in New Haven, Conn. These teams include many experts who each play a role in the care of patients with pancreatic NETs, such as medical oncologists, surgical oncologists, pathologists, radiologists, nuclear medicine specialists, endocrinologists and others.




 Like the DIY idea of Dr. Leonardo websites, but just don’t want to Do-It-Yourself? We understand! Fussing over website details isn’t for everyone. But we do love building websites with our builder and we’re kind of obsessive about how we do things. Plus, we can build them lickety-split – typically in
Like the DIY idea of Dr. Leonardo websites, but just don’t want to Do-It-Yourself? We understand! Fussing over website details isn’t for everyone. But we do love building websites with our builder and we’re kind of obsessive about how we do things. Plus, we can build them lickety-split – typically in